Anaphylaxis Policy

Introductory Statement
This policy is concerned with the whole school approach to the health care and management of members of the school community suffering from serious specific allergies.
The school’s position is not to guarantee a completely allergen free environment. Our aim is to minimise the risk of exposure, encourage self-responsibility, plan for effective response to possible emergencies and become an ‘allergy aware’ environment. The school recognises that a number of community members suffer from potentially life-threatening allergies to certain foods, or toxins from peanuts, nuts and eggs.
Rationale
The intent of this policy is to:
- Identify risks for anaphylaxis.
- Minimise the risk of any student suffering allergy induced anaphylaxis whilst at school or attending any school related activity.
- Ensure staff are properly prepared to manage such emergency situations should they arise.
Definitions
Allergy: A condition in which the body has an exaggerated response to an allergen.
Allergen: A normally harmless substance that triggers an allergic reaction in the immune system of a susceptible person.
Anaphylaxis or anaphylactic shock: A sudden, severe and potentially life-threatening allergic reaction to food, stings, bites, or medicines.
Adrenaline Autoinjector: A medical device for injecting a measured dose or doses of adrenaline by means of autoinjector technology. A number of brands used include Emerade®, EpiPen®, Jext®
Anaphylaxis Action Plan: A clear document with information on how to recognise anaphylaxis and how to administer the child’s adrenaline autoinjector and emergency contact details.
Guidelines
The school’s key guidelines are to:
- Identify the student with the food allergy in the school.
- Have a written Anaphylaxis Action Plan for each child at risk of anaphylaxis. This plan must be written by child’s doctor and parents.
- The avoidance to allergens followed at home should be applied to the classroom.
- There is a ‘no share food’ policy in relevant classroom.
- Where food is consumed, the following must be in place:
- hand washing (In so far as possible)
- no food sharing
- routine cleaning of surfaces where food is consumed to avoid cross contamination
- Every student with life-threatening allergies must have two pairs of medically prescribed adrenaline autoinjectors in the school.
The adrenaline autoinjectors (2 autoinjectors) need to be accessible for quick access within 1-2 minutes of a reaction and therefore will be kept in a first aid bag in the classroom with the class teacher in An Anaphylaxis Emergency Kit. A second set of two autoinjectors will be available in an unlocked, accessible location beside the school office.
Commitment
The School is committed to proactive risk allergy management through:
- The encouragement of self-responsibility and learned avoidance strategies amongst students suffering allergies (age appropriate).
- Provision of staff education / training programme on anaphylaxis.
- The establishment of specific risk exposure minimisation practices and strategies wherever required within the School operations.
- Close liaison with parents of students who suffer allergies.
The adrenaline autoinjectors (2 autoinjectors) need to be accessible for quick access within 1-2 minutes of a reaction and therefore will be kept in a first aid bag in the classroom with the class teacher in An Anaphylaxis Emergency Kit. A second set of two autoinjectors will be available in an unlocked, accessible location beside the school office.
School Responsibility
- Follow the procedures laid out in this policy.
- Understand the causes, symptoms and treatment of anaphylaxis. Be able to recognise symptoms, know what to do in an emergency, be prepared to handle an allergic reaction.
- Be aware of the students in their care who are at risk from such reactions.
- Review and be aware of the Anaphylaxis Action Plan for the pupil.
- Implement a ‘No share policy’ in the child’s classroom.
- Accessibility of each Anaphylaxis Emergency Kit: The Adrenaline injectors in each of the two Anaphylaxis Emergency Kits should always be accessible – never in a locked room or cupboard. Injectors are normally stored at room temperature out of direct sunlight and away from radiators. Manufacturer’s storage guideline should be followed.
- Ensure that the pupil’s Anaphylaxis Emergency Kit is readily accessible.
- Each kit must be kept in a place where it can be clearly seen and accessed by a trained staff member (one in the pupil’s classroom and one in a central location in the school).
- Where food treats are used in class the child will be rewarded with treats provided by parent.
- Ensure that tables and surfaces are kept clean regularly and that students are encouraged to wash their hands before and after handling food.
- Discuss activities involving food with parents/guardians before they take place and arrange for the provision by the parents/guardians of alternative options for edible treats on special occasions.
- Provide information for substitute teachers, and communicate the day-to-day needs of the pupil with allergies and the Anaphylaxis Action Plan.
- Ensure the pupil’s Anaphylaxis Emergency Kit (pens and anti-histamine) and a mobile phone is taken on all outings and trips off the school premises.
- Become familiar with the concept of "hidden" ingredients, not only in foods but also in non-food items that may be used in classroom projects in arts and crafts (e.g. egg boxes may contain trace egg shells), science (presence of nuts in bird feeders and nature tables). Reading the ingredient labels of foods, as well as other items becomes an additional responsibility of the class teacher.
- Be aware that students are at most risk when:
- Their routine is broken, children being moved to another classroom.
- At yard or during eating times.
- On school tours immediate access to medical services is not available.
- Staff changes occur (sub teacher etc.) .
- Participating in activities involving food, e.g. bake sale.
NOTE
It is extremely important that staff follow the ‘Anaphylaxis Action Plan’ procedure to the letter, and administer the adrenaline autoinjectors in any situation where symptoms show the need.
If there is any doubt about whether to give Adrenaline or not, the medical consensus is GIVE IT. In a scenario where anaphylaxis is possible, a student is better off receiving adrenaline (even if in retrospect it wasn’t required) than not. Allergy doctors agree it is wiser to over-react than to under react.
St. Patrick’s BNS, Hollypark will adopt this best practice on medical advice.
Every Family’s Responsibility
- Be allergy aware.
- Teach their children to eat out of their lunchbox.
- Support the school in the implementation of this policy.
Child with Allergies, Family’s Responsibility
- Notify the school of the child’s allergies on diagnosis on enrolment. Provide the Principal with an immediate update if there is a change to their child’s condition.
- Provide written medical documentation, instructions and medications as directed by a physician, using the Anaphylaxis Action Plan so that staff will know how to react should their child have an allergic reaction.
- Provide the school with the contents for two Anaphylaxis Emergency Kits. Each kit should include two adrenaline autoinjectors, the Anaphylaxis Action Plan(by email), antihistamines and inhalers if required. The school will provide the special storage bags for these Anaphylaxis Emergency Kits and they will be labelled clearly with pupil’s name, and a photograph of the pupil. Each kit must be kept in a place where it can be clearly seen and accessed by a trained staff member -one in the pupil’s classroom and one in a central location in the school.
- Parents/guardians are responsible for checking expiry dates of all medication and should replace them as necessary. The ideal time to do this is at the end of each term.
- Parents/guardians must also ensure, with their doctor, that the dose prescribed is adequate and be aware this changes as dictated by the weight of the child.
- Supply alternative food options for their child when needed, e.g. on Pancake Tuesday (the school will give advanced notice of events such as these).
- Support the school in the implementation of this policy.
- Educate the child in self-management of their food allergy including safe and unsafe foods to eat.
- Strategies for avoiding exposure to unsafe foods.
- Symptoms of allergic reactions.
- How and when to tell an adult they may be having an allergy related problem (age appropriate).
- How to read food labels (age appropriate).
- Provide emergency contact information and inform the school if this information changes.
- Review procedure with the school staff, child’s doctor and the child (if age appropriate) after a reaction has occurred.
Child with Allergies Responsibility
- Should not trade food with others – no share policy.
- Should not eat anything with unknown ingredients or known to contain an allergen.
- Should notify an adult immediately if they eat something, they believe may have contained the food to which they are allergic (age appropriate).
- Should notify an adult immediately if they feel they are beginning to get an allergic reaction.
Raising Student & Parent Awareness
It is important to work with the whole school community to better understand how to provide a safe and supportive environment for all students, including the student with severe allergies. Peer support and understanding is important for the student at risk of anaphylaxis. The following key messages should be given to children in an age appropriate manner.
- Take allergic reactions seriously – serious allergies are no joke
- Don’t share your food with your classmates
- Not everyone has allergies – discuss common symptoms
- Wash your hands before and after eating
- Know what your friends are allergic to
- If a schoolmate or teacher becomes sick, get help immediately
- Be respectful to all school friends
Food allergic children are known to experience considerable anxiety due to their condition. They suffer limitations, isolation and exclusion every day. The School will provide positive psychosocial environment ensuring inclusion and acceptance. Parents will be made aware of this policy on the enrolment of a child with anaphylaxis or when newly enrolled.
Review Management Strategies
If a student has experienced an anaphylactic shock
- The child’s adrenaline autoinjector must be replaced by the parents.
- The school together with parents will review the Anaphylaxis Action Plan (the child’s doctor’s input would be necessary at this time).
Procedure During a Severe Allergic Reaction
The pupil’s Anaphylaxis Action Plan forms an important part of the school’s risk management plan and will enable any situation to be managed promptly and efficiently. All staff should be familiar with this plan and the procedures to be followed in the event of an emergency.
NOTE
Delays in giving emergency medication or contacting emergency services can result in serious and rapid deterioration in an anaphylactic pupil’s condition, therefore the priority actions are to treat the pupil immediately and phone emergency services
What to Do in an Emergency
If a student with allergies shows any possible symptoms of a reaction, immediately seek help from a member of staff trained in anaphylaxis emergency procedures
- The trained member of staff should assess the situation
- Administer appropriate medication in line with symptoms. If symptoms suggest it is a severe reaction, the trained member of staff should give the pupil their Adrenaline auto-injector into the outer aspect of their thigh.
- Send for the immediate support of another staff member(s).
- If there is no improvement after 5 minutes the trained member of staff should: Give the second Adrenaline auto-injector.
- Continue to assess the pupil’s condition.
- Position the pupil in the most suitable position according to their symptoms.
- The support staff member should call for an ambulance and call the pupil’s parents
Sample Anaphylaxis Action Plan
Mild to Moderate Reaction
- Tingling of lips face, eyes
- Hives or rash
- Abdominal pain, vomiting

Action
- Stay with child
- Call for help
- Give 10mls of antihistamine

Watch for signs of ANAPHYLAXIS
- Swelling of lips, tongue
- Rash/hives suddenly
- Throat tightness
- Difficult/noisy breathing
- Hoarse voice/altered cry
- Wheeze/cough
- Pale/floppy
- Collapse/decreased consciousness

If any of these symptoms occur
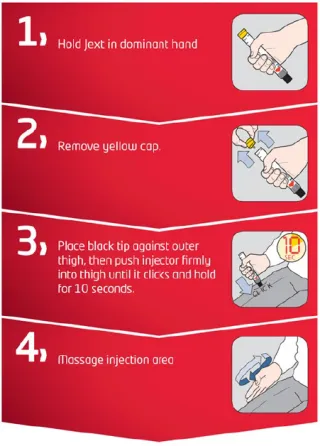
- Give adrenaline autoinjector
- Call 99 immediately
- Lie child down and raise legs
- If he has not improved in 5 minutes repeat adrenaline
IF IN DOUBT GIVE ADRENALINE
This policy was formulated by the Staff of Hollypark B.N.S. in consultation with the Parents and Board of Management.
Created March 2021
Ratified by the Board of Management
Chairperson, Board of Management
Date: March 2021
Next review March 2022